This activity is supported by educational grants from Abbott Cardiovascular, AstraZeneca US, Bayer AG, and Novo Nordisk.
In case you missed the Journal Club in Twitter “real time” you can review the course material here and earn the same credit.
Welcome to our first accredited Twitter Journal Club! Each earns 0.5h credit for docs, nurses, pharmacists. Starting tomorrow, learn about insertable cardiac monitors. @academicCME #cardiotwitter #medtwitter
1/
Welcome to Journal Club! This program is accredited for 0.5h CE credit. Complete it and then follow directions (in next Thursday’s final tweet in this series) for claiming credit. So easy! This program supported by grants from Abbott and Bayer. Ready to go???
2/
Prolonged rhythm monitoring with a SQ insertable cardiac monitor (ICM) is of diagnostic value in patients with unexplained recurrent syncope. DDx includes unproven epilepsy, unexplained falls, and other arrhythmias.
3/
2018 ESC Guidelines suggest ICM instead of an ICD in many patients with recurrent unexplained syncope and low risk of SCD. ICM may be esp useful in different those with neurally mediated syncope, BBB, or structural heart disease–more so than tilt table or Holter.
4/
Currently available ICMs:
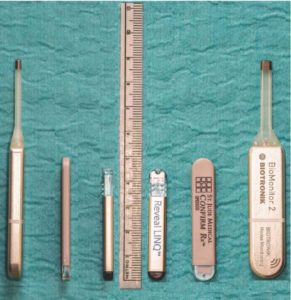
5/
In CARISMA, 297 patients with LVEF≤40% 3-21d post-AMI were followed with an ICM for (mean) 1.9y. Arrhythmias documented: new-onset AF (28%), non-sustained VT (13%), high-degree AV block (10%). Which of these was strongest predictor of cardiac death?
POLL: (a) new-onset AF, (b) non-sustained VT, (c) high-degree AV block
6/
High-degree AV block was the most powerful predictor of cardiac death. Nonetheless, guidelines currently don’t recommend routine ICM post-MI, unless patients have recurrent unexplained syncope with systolic impairment and don’t have a current indication for an ICD.
7/
REVISE study: 103 pts with epilepsy but likely misdiagnosed. Enrolled if 3/+transient LOC episodes in yr before enrol. ICM recorded profound bradyarrhythmia or asystole with convulsive features in 21%, who were offered pacemaker. After pacing and d/c sz meds, 60% became asx.
8/
ESUS cryptogenic stroke: a good indication for ICM, as recurrence is common and AF detection might allow treatment. Intermittent monitoring (annual 24h or quarterly 7d Holter) for AF inferior to cont ICM. ICMs shown to be a cost-effective dx’ic tool for sec prevention in ESUS.
9/
Stroke prevention: a high incidence of subclinical AF in high-risk populations demonstrated using ICMs. Not clear if SCAF conveys same thromboembolic risk as clinical AF, but incidence of SCAF detected in high-risk cohorts, at 1y monitoring time, was:
POLL: (a) 10-20%, (b) 20-30%, (c) 30-40%, (d) 40-50%
10/
SCAF detection was 20-31%. REACT.COM tested ICM-guided intermittent NOAC admin in pts w/nonperm AF+CHADS2=1 or 2. Plan? That cont ICM monit + rapid onset of NOAC allowed targeted AC only around an AF episode (≥1 h). Result: 94% ↓ in time on NOAC, no strokes.
11/
ICMs evolving to allow early detection of HF. Expanding market of medical wearables may compete, but have disadvantages over implanted device for continuous monitoring. Miniaturization, reliable data transmission, and ↑ capabilities = bright future for ICMs.
Please complete the evaluation below and claim your 0.5 CE Credit.